The Lymphatic System: An Anatomical Deep Dive
The lymphatic system is a complex network of vessels, nodes, and organs responsible for fluid balance, immune surveillance, and waste filtration. Unlike the cardiovascular system, it does not have a central pump. Its flow depends entirely on pressure gradients, movement, and structural design.
Understanding its anatomy explains why swelling happens, why fluid retention occurs, and why directional support matters.
Let’s break it down properly.
The Structural Components of the Lymphatic System
The lymphatic system is made up of four main anatomical components:
- 1. Lymphatic capillaries.
- 2. Lymphatic vessels
- 3. Lymph nodes
- 4. Lymphatic ducts and associated organs
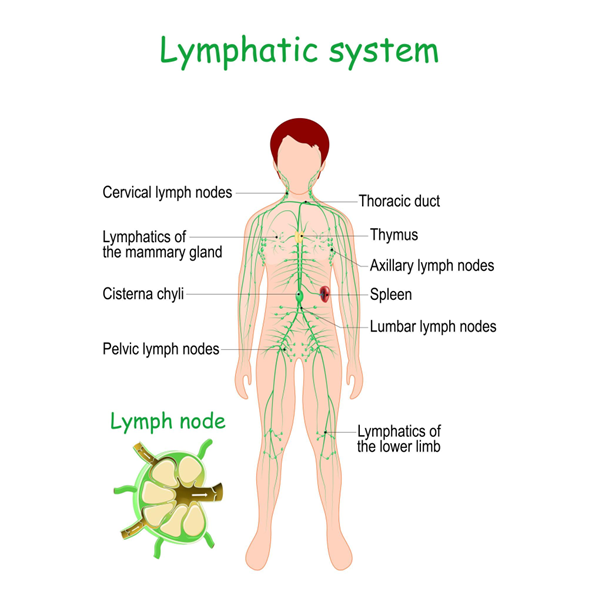
Each plays a specific role in fluid transport and immune regulation.
- 1. Lymphatic capillaries - Where it Begins
- Lymphatic circulation starts at the tissue level. Throughout your body, tiny blood capillaries constantly leak small amounts of plasma into surrounding tissues. This fluid nourishes cells but must be reabsorbed. Some returns directly to veins.
- The rest enters lymphatic capillaries. These capillaries are:
- Blind-ended (they start in tissues)
- Extremely thin-walled
- Highly permeable
- Their structure allows them to absorb:
- Excess interstitial fluid
- Proteins
- Cellular debris
- Bacteria
- Viruses
- Once inside these capillaries, the fluid is now called lymph. This is the first stage of lymphatic circulation.
- 2. Lymphatic Vessels – The Transport Network
- From the capillaries, lymph moves into progressively larger vessels. Lymphatic vessels resemble veins in structure. They contain:
- Thin muscular walls
- One-way valves
- Segmental chambers called lymphangions
- These valves are critical. They prevent backflow and ensure lymph moves in one direction — toward the central circulation. Unlike arteries, there is no heart pumping lymph forward. Movement occurs through:
- Skeletal muscle contraction
- Respiratory pressure changes
- Arterial pulsation
- External mechanical stimulation
- This explains why immobility slows lymph flow.
- 3. Lymph Nodes – The Filtration Stations
- Lymph nodes are small, bean-shaped structures located along lymphatic pathways. Major clusters exist in:
- Cervical region (neck)
- Axillary region (armpits)
- Inguinal region (groin)
- Abdomen and pelvis
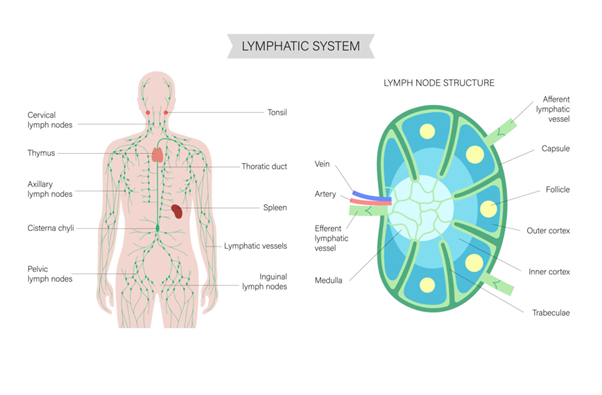
- Anatomically, each node contains:
- An outer cortex (rich in B lymphocytes)
- A paracortex (rich in T lymphocytes)
- A medulla (containing macrophages and plasma cells)
- When lymph enters a node, it slows down. This allows immune cells to:
- Detect pathogens
- Destroy foreign particles
- Activate immune responses
- This is why lymph nodes swell during infection — they are actively filtering and responding. Nodes are not random. They are strategically positioned along drainage pathways.
- 4. The Lymphatic Ducts – Final Drainage Pathways
- All lymph eventually drains into two major ducts:
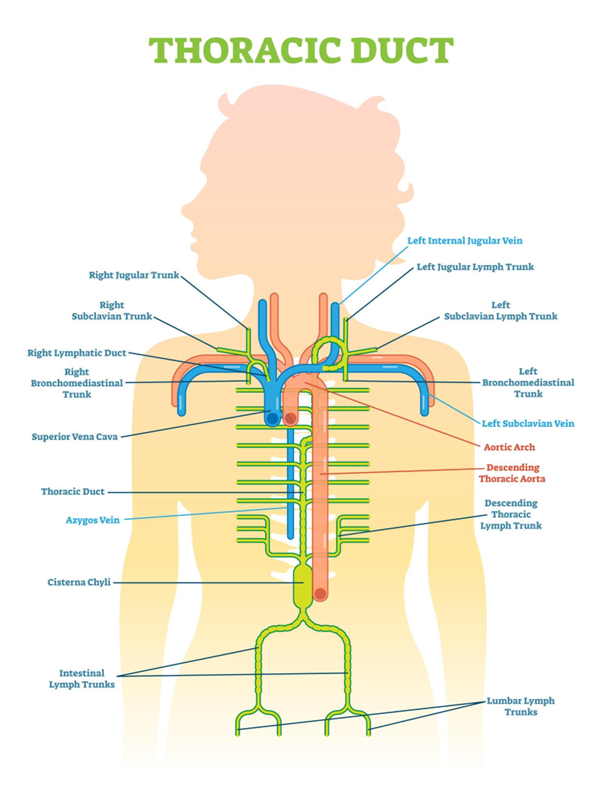
- The Thoracic Duct - the largest lymphatic vessel in the body. It collects lymph from:
- Both legs
- Abdomen
- Left arm
- Left side of the head and chest
- It empties into the left subclavian vein.
- The Right Lymphatic Duct drains:
- Right arm
- Right side of head and neck
- Right side of chest
- It empties into the right subclavian vein. This anatomical asymmetry explains why swelling patterns can vary depending on region. Once lymph re-enters the bloodstream, it rejoins normal circulation.
The Flow Dynamics of the Lymphatic System
Unlike the cardiovascular system, the lymphatic system operates under low pressure.
Flow depends on:
- Pressure gradients
- Valve integrity
- Muscle contraction
- Tissue compression
If any of these are compromised — such as after surgery, trauma, or prolonged inactivity — lymph flow can slow. When lymph accumulates in tissues, it causes:
- Oedema (swelling)
- Heaviness
- Tissue tightness
- Reduced mobility
The anatomical design means that flow must follow a specific directional pattern toward central ducts. This directional anatomy is important when applying structured lymphatic techniques.
Lymphatic Territories and Drainage Pathways
The body is divided into lymphatic “watersheds.” These are imaginary lines that separate drainage territories. For example:
- The umbilical line divides upper and lower body drainage
- The midline divides left and right drainage
Lymph does not randomly cross these boundaries. It follows predictable anatomical routes toward regional nodes. This is why understanding drainage patterns is crucial when attempting to influence lymph movement.
Associated Lymphatic Organs
Beyond vessels and nodes, the lymphatic system includes:
- The Spleen - Filters blood and recycles red blood cells.
- The Thymus - Located behind the sternum; essential for T-cell maturation during early life.
- Tonsils and Adenoids - Provide immune surveillance at entry points of the respiratory tract. These organs support immune function but do not directly transport lymph in the same way vessels do.
What Happens When the System Is Overloaded?
When lymph production exceeds drainage capacity, swelling occurs. Common triggers include:
- Surgical tissue disruption
- Soft tissue injury
- Inflammation
- Infection
- Reduced mobility
- Hormonal fluid shifts
If drainage pathways are obstructed or overwhelmed, fluid remains in interstitial spaces. This creates:
- Pressure
- Discomfort
- Slower healing
- Increased inflammatory response
The anatomical explanation makes it clear: the system must move fluid directionally and sequentially to function effectively.
Why Anatomical Precision Matters
Because the lymphatic system is directional and valve-based, stimulating it requires understanding:
- Node Locations
- Drainage order
- Regional watershed boundaries
- Central clearance pathways
Stimulating peripheral areas without first clearing central nodes may reduce efficiency. The system is not random. It is organised, structured, and anatomically mapped.
Understanding this is the difference between generic pressure and structured lymphatic support.
The Bigger Picture
The lymphatic system is not just about swelling. It is a fundamental regulatory system involved in:
- Immune Defence
- Inflammation control
- Fluid equilibrium
- Tissue recovery
It quietly processes litres of fluid every day. It filters pathogens. It manages inflammatory by-products. And it relies heavily on movement and anatomical integrity to function optimally.
When you understand its structure — capillaries, vessels, nodes, ducts — you begin to see why fluid retention occurs, why post-surgical swelling behaves the way it does, and why proper directional support must follow anatomy. The lymphatic system is subtle. But it is foundational.
Gentle Care, Powerful Healing.
Book your lymphatic drainage massage with our expert therapists at Interactive Therapies in Auckland.
We’ll assess your body, explain the options, and help you start a treatment plan that’s right for you.
Anatomical FAQs: The Lymphatic System
What is the difference between lymphatic vessels and blood vessels?
Blood vessels operate under high pressure and are powered by the heart. Arteries carry blood away from the heart, veins return it, and capillaries allow nutrient exchange.
Lymphatic vessels, on the other hand, operate under very low pressure. They do not have a pump. Instead, they rely on skeletal muscle movement, breathing mechanics, and one-way valves to move lymph fluid toward the central ducts.
Structurally, lymphatic vessels resemble veins but are thinner and more permeable. They contain internal valves that prevent backflow. When these valves function properly, lymph moves directionally toward the thoracic duct or right lymphatic duct.
Because the system depends on external movement, immobility or tissue disruption can significantly slow lymph transport.
Why does swelling occur if lymphatic vessels are intact?
Swelling (oedema) occurs when the volume of interstitial fluid exceeds the lymphatic system’s drainage capacity. Even if vessels are anatomically intact, swelling may happen due to:
- Increased capillary leakage (inflammation or trauma)
- Reduced muscle activity
- Temporary blockage from surgical disruption
- Overwhelmed lymph nodes
The system can usually manage normal fluid loads. However, after injury or surgery, fluid production increases significantly. If drainage pathways cannot keep up, fluid accumulates in tissues. This is why post-surgical swelling can persist even without structural damage to vessels.
What is the thoracic duct and why is it important?
The thoracic duct is the largest lymphatic vessel in the body. It collects lymph from:
- Both lower limbs
- Abdomen
- Left side of the chest
- Left arm
- Left side of the head and neck
It empties into the left subclavian vein, where lymph re-enters the bloodstream. Because it drains such a large portion of the body, central congestion near the thoracic duct can influence widespread fluid retention.
Anatomically, effective lymph movement requires that central pathways remain unobstructed before peripheral regions are stimulated.
Can lymph nodes regenerate or repair themselves?
Lymph nodes contain active immune tissue and can respond dynamically to stress, infection, or inflammation. They can enlarge temporarily when fighting infection due to immune cell proliferation.
However, if lymph nodes are surgically removed or significantly damaged, drainage pathways may be permanently altered. The body can sometimes compensate by using collateral pathways, but these are not always as efficient as original structures.
This anatomical reality explains why directional lymphatic support is often discussed in post-surgical contexts.
Further Reading: Understanding the Lymphatic System & Swelling
- Lymphatic Drainage & Post-Surgical Swelling: Anatomy Explained. Learn how lymphatic vessels respond after surgery and why swelling occurs during recovery.
- The Complete Guide to Lymphatic System Swelling. A comprehensive overview of causes, symptoms, and management strategies for lymphatic-related swelling
- Lymphatic Drainage Massage: The Anatomy Behind It A detailed look at how manual lymphatic drainage techniques interact with lymph vessels and nodes.
- Fluid Retention vs. Lymphatic Congestion: What’s the Difference? Understand how to distinguish between general water retention and true lymphatic stagnation.
- Lymphatic Drainage: Common Myths Explained. Separate fact from fiction about detox, massage, and how the lymphatic system actually works.
Post Related
Unveil Your Most Beautiful Self.
Refine
Body
Face
Services
Follow us on :
Copyright © 2025 Interactive Therapies (2025) Ltd | Powered by Business Squad



